Rocky Mountain Spotted Fever — RMSF
Reviewed by: Joel Klein, MD and Clifton Castleman, WEMT & lead acarologist at TickSafety.com
Jared spends most weekends hiking in the foothills of the wooded mountains near his home. Just days after one of these hikes, he suddenly woke up with a high fever, aching muscles, chills, and a bad headache. He thought he was getting the flu, but then a few days later, he started getting a spotted red rash on his wrists and ankles.
Jared, who’s pretty savvy about the outdoors, wondered if his illness had anything to do with the ticks he’d seen in the thick grasses and bushes along the trails. A trip to the doctor confirmed his guess – Jared had Rocky Mountain spotted fever.
What Is Rocky Mountain Spotted Fever?
Rocky Mountain spotted fever (or RMSF for short) is a disease caused by infection with Rickettsia rickettsii (R. rickettsii), a type of bacteria. R. rickettsii are usually carried by ticks: Most people who develop RMSF do so after being bitten by one of two types of ticks – the American Dog tick in the eastern and central United States, and the Rocky Mountain Wood tick in the Rocky Mountain states and southwestern Canada.
The bacteria that cause the infection are transmitted to humans by tick bites, so RMSF occurs most often when ticks are active. More than 90% of RMSF cases happen between April and early September, and occur (of all places) East of the Mississippi River (in Virginia, in particular).
Studies show that less than 3% of ticks actually carry R. rickettsii, so getting a tick bite doesn’t automatically mean someone will be exposed to the bacteria or get RMSF. About 500 to 600 infections are reported in the United States each year; most of these cases occur in children.
A person doesn’t have to actually live in or near the Rocky Mountains to get RMSF. In fact, according to the Centers for Disease Control and Prevention (CDC), there have been cases of RMSF in all parts of the United States (with the exception of Alaska, Hawaii, and the northern New England states). It is most common in the southeastern states that border the Atlantic Ocean (Virginia, the Carolinas, and Georgia) and westward into states like Tennessee, Arkansas, and Oklahoma.
The bacteria that cause RMSF are transmitted from a tick to a person while the tick is attached to the person’s skin. When a tick bites someone, it is actually preparing to stay attached for a while to feed on the person’s blood.
If a tick is infected with R. rickettsii, the longer that tick stays attached, the more likely it is to transmit the bacteria through its mouth into the person’s blood. Usually several hours are needed for this to occur. During this time, the tick will become swollen with blood from feeding. Swollen ticks usually appear grayish and bloated.
It’s also possible for a person to get RMSF if that person has a cut or blister that comes into contact with body juices from a crushed tick. This is why it’s important never to crush a tick with your fingers while removing it. Handling ticks with bare hands isn’t a good idea. Use a tissue or non-latex gloves whenever possible.
Signs and Symptoms of RMSF
 The symptoms of RMSF generally appear within 2 to 14 days of a tick bite. In many cases, people who get RMSF aren’t even aware that a tick bit them. For many people, symptoms of RMSF begin suddenly, although this isn’t always the case: About a third of all people with the infection notice that their symptoms appear gradually. Symptoms include a flu-like feeling, such as fever, chills, fatigue, muscle aches, and severe headache. A person may also experience abdominal pain, nausea, vomiting, and diarrhea and may not feel like eating.
The symptoms of RMSF generally appear within 2 to 14 days of a tick bite. In many cases, people who get RMSF aren’t even aware that a tick bit them. For many people, symptoms of RMSF begin suddenly, although this isn’t always the case: About a third of all people with the infection notice that their symptoms appear gradually. Symptoms include a flu-like feeling, such as fever, chills, fatigue, muscle aches, and severe headache. A person may also experience abdominal pain, nausea, vomiting, and diarrhea and may not feel like eating.
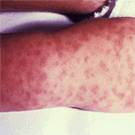
Days later, a person with RMSF may develop a skin rash that looks like small pinkish-red or dark red spots or blotches. The rash often appears 2 to 5 days after other symptoms start. It typically begins on the wrists, ankles, palms, and soles of the feet and then spreads up the arms and legs toward the chest, belly, and back. As RMSF progresses, the original red spots may change in appearance to look more like bruises or bloody dots or patches under the skin. A few people with RMSF don’t get any type of rash, though.
RMSF can be severe. In severe cases, the blood vessels, liver, kidneys, intestines, lungs, or brain can all be affected by the illness and may become damaged. So it’s important to see a doctor if you think you have the signs and symptoms of RMSF.
How Do Doctors Diagnose RMSF?
Even if you’re not sure whether a tick may have bitten you, you should call your doctor if you have any symptoms of RMSF like fever, headache, chills, muscle aches, and rash, especially if the rash starts around your ankles and wrists.
To diagnose RMSF, a doctor will usually take several blood tests, and at least two different blood samples (several weeks apart) to look for rising antibodies against the infection. Antibodies are special proteins made by the body to help fight specific infections.
Because it may take several days for blood tests to show positive results, your doctor will probably begin treatment before test results are available if he or she suspects you have RMSF based on your symptoms.
How Is It Treated?
RMSF is treated with antibiotics. Someone with a mild case of the infection can be treated at home, but some patients who are more seriously ill need to be treated in the hospital with intravenous (IV) antibiotics and fluids. When medicines or fluids are given intravenously, they are placed directly into the bloodstream through a needle that goes into a person’s vein.
Treatment with antibiotics usually continues until a person with RMSF is no longer feeling ill and the fever goes down. Most treatments for RMSF last for 7 to 10 days. If there are complications from RMSF, such as continued fever or signs of inflammation in the body, treatment will last longer.
It’s very important for anyone who may have RMSF to get treated quickly and to follow the doctor’s instructions for taking all medicines and recovering at home. That’s because the infection can be serious – and in rare cases even fatal – if it’s not treated.
Can I Prevent It?
RMSF is not contagious from person to person, so you can’t catch it from someone who has it. At present, there is no vaccine available to prevent infection with RMSF.
The best way to avoid getting RMSF is to avoid tick-infested areas. Ticks like to hang out in grassy and wooded areas. But if you enjoy doing activities in the wooded outdoors such as hiking or camping, know how to protect yourself from ticks:
- Try to wear light-colored clothing that makes ticks more visible if they are crawling on you. This can help you see ticks before they latch onto your skin.
- Use an insect repellent that works for ticks and contains 10% to 30% DEET (N,N-diethyl-m-toluamide), being careful to follow label directions carefully.
- Wear long-sleeved shirts and long pants and tuck your pant legs into your socks.
- Check for ticks on your body at least once each day and before going to bed. Don’t overlook a tick’s favorite hiding places: the scalp, behind the ears, under the arms, on the ankles, and in the groin or genital areas. The CDC recommends using a handheld mirror to check these places if they are difficult to see.
- Wash your clothes and hair after leaving tick-infested areas.
If you find a tick on your body, remove it immediately. If it is difficult to remove, ask someone to help you.
Even if you don’t go into areas where ticks live, your dog or cat might! Because pets can bring ticks into your home, check their skin and fur for ticks whenever they have been playing in areas that may be infested with ticks. Ticks can jump off pets to bite and feed on humans instead. Follow your veterinarian’s advice about collars and other products that can be used to keep your pet tick free.


